Anxiety & Depression
The National Comorbidity Survey reported that 46% of men and 58% of women will suffer at least a two week period in their lifetime, in which they experience a persistent depressed mood. Major depression disorder (MDD) has a lifetime prevalence of about 16%, and post 2020, it is the second greatest contributor to the impairment of global health. A recent Australian survey reported that anxiety disorders were the most common mental disorder with a lifetime prevalence of 26%.
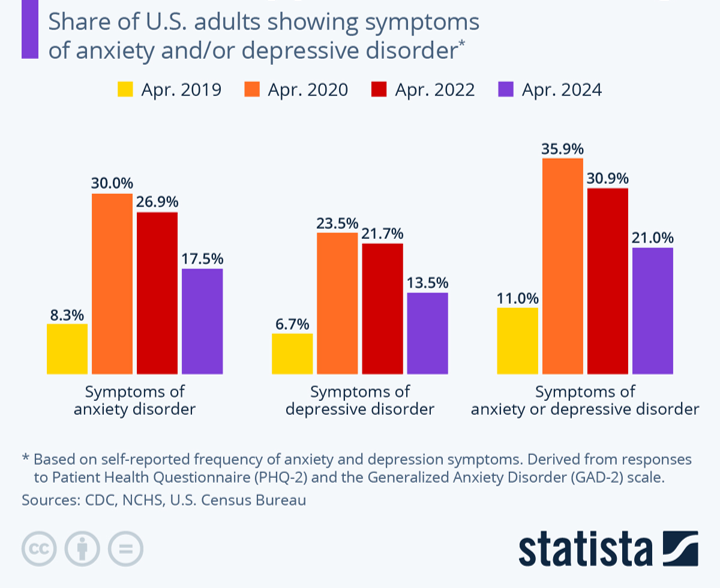
According to Felix Richter: Aside from killing 1.2 million Americans, putting millions in the hospital and wreaking havoc on the country’s economy, the Covid-19 pandemic also took a heavy toll on mental health. Data compiled by the U.S. Census Bureau and the National Center for Health Statistics clearly showed a spike in the prevalence of symptoms associated with anxiety and/or depressive disorder following the onset of the pandemic. These psychologial effects of Covid-19 even outlived the pandemic itself, as in March/April 2024, symptoms of anxiety or depression were still roughly twice as common as they were in April 2019.
The Department of Psychiatry, Harvard Medical School and the Laboratory for Psychiatric Biostatistics, McLean Hospital
According to Paula Askalsky & Dan V Iosifescu, from the Department of Psychiatry, NYU Langone School of Medicine, New York, USA: Major depressive disorder (MDD) is prevalent (affecting 16.2% of the US population, lifetime) and disabling, being among the leading causes of years lived with disability worldwide. Existing antidepressants have burdensome side effects and are only partially effective; more than one-third of MDD patients do not achieve remission after several adequate antidepressant trials, and relapses are frequent.3 One option for individuals who do not respond to or tolerate antidepressant medications are neuromodulation strategies….BUT…studies reviewed, using photobiomodulation provide strong evidence for the mechanism of t-PBM (increasing mitochondrial energy production and increasing regional blood flow). The downstream effects of increased ATP production include not only increased cellular energy but also potentially increases in intercellular signalling…with positive effects on anxiety and depression treatment.
